Genetic evidence for a potential causal relationship between insomnia symptoms and suicidal behavior: a Mendelian randomization study
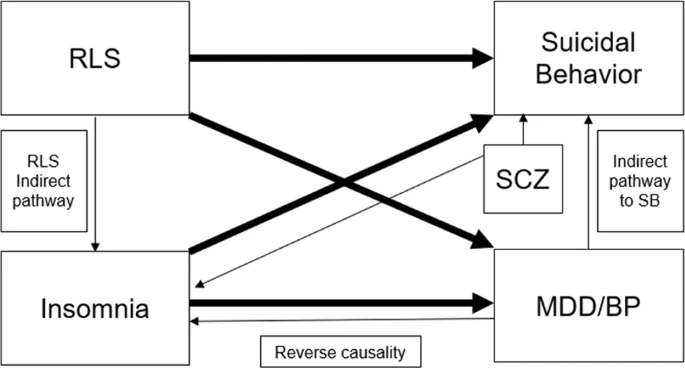
Insomnia and restless leg syndrome (RLS) are associated with increased risk for suicidal behavior (SB), which is often comorbid with mood or thought disorders; however, it is unclear whether these relationships are causal. We performed a two-sample Mendelian randomization study using summary-level genetic associations with insomnia symptoms and RLS against the outcomes of risk of major depressive disorder (MDD), bipolar disorder (BP), schizophrenia (SCZ), and SB. The inverse-variance weighted method was used in the main analysis. We performed replication and sensitivity analyses to examine the robustness of the results. We identified outcome cohorts for MDD (n = 170,756 cases/329,443 controls), BP (n = 20,352/31,358), SCZ (n = 69,369/236,642), SB-Cohort-2019 (n = 6569/14,996 all with MDD, BP or SCZ; and SB within individual disease categories), and SB-Cohort-2020 (n = 29,782/519,961). Genetically proxied liability to insomnia symptoms significantly associated with increased risk of MDD (odds ratio (OR) = 1.23, 95% confidence interval (CI) = 1.2-1.26, P = 1.37 × 10-61), BP (OR = 1.15, 95% CI = 1.07-1.23, P = 5.11 × 10-5), SB-Cohort-2019 (OR = 1.17, 95% CI = 1.07-1.27, P = 2.30 × 10-4), SB-Cohort-2019 in depressed patients (OR = 1.34, 95% CI = 1.16-1.54, P = 5.97 × 10-5), and SB-Cohort-2020 (OR = 1.24, 95% CI = 1.18-1.3, P = 1.47 × 10-18). Genetically proxied liability to RLS did not significantly influence the risk of any of the outcomes (all corrected P > 0.05). Results were replicated for insomnia with MDD and SB in Mass General Brigham Biobank and were consistent in multiple lines of sensitivity analyses. In conclusion, human genetic evidence supports for the first time a potentially independent and causal effect of insomnia on SB and encourages further clinical investigation of treatment of insomnia for prevention or treatment of SB.

